
| T H E N I H C A T A L Y S T | M A R C H - A P R I L 2000 |
|
|
|
ELAINE JAFFE: HERCULE POIROTIN A PATHOLOGICAL UNIVERSE |
by Cynthia Delgado |
One of the world’s most called-upon resources in the field of hematopathology resides in NCI’s Laboratory of Pathology, where she serves as deputy chief and from where she responds to distant calls for help, unravelling the diagnostic dilemmas sent to her by clinicians the world over and by patients seeking impartial advice on treatment options.
 |
|
Elaine Jaffe at
her window
on the world of disease
|
Last year, the Institute for Scientific Information released survey results, reported in the May-June 1999 issue of Science Watch, that named Elaine Jaffe among the 100 most-cited researchers in clinical medicine and among the top 10 in oncology between the years 1981 and 1998. She was the only female clinician listed, which she sees predominantly as a reflection of the realities of the years covered in the survey. "Back in 1981," she says, "there were fewer women in the field and fewer women publishing. I would hope that if we did a survey from, let’s say ’90–’98, there would be many more women included." Asked if being a woman in science had presented any particular challenges to her research, she replies, "Not really." And asked to what she attributes her success, she credits the "unique scientific environment of NCI."
In an interview with The
NIH Catalyst,
Jaffe elaborated on
the advances in immunology and molecular genetics that have transformed the
tools of pathologic diagnosis and the classification systems for lymphomas
and leukemias and, with unfolding microarray technology, the molecular disease
profile of all cancers.
She emphasized the clinical context of pathological findings, without which
the
disease entity may fail to be appreciated and optimal management may remain
elusive.
And she sang the praises
of the contributions and rewards of her profession. Far from being
"locked in a morgue," as the public may perceive them, pathologists
perform exquisite detective
work that uncovers disease mysteries and helps keep people alive and healthy.
The interview follows.
Q: What lured you into the study of pathology?
JAFFE: During medical school, I came to realize I was very interested in the process and the pathogenesis of disease and less interested in dealing with patients on a one-on-one basis. It was the pathology course I took as a second-year medical student that was pivotal; it was then that I saw pathology as laying the groundwork for the understanding of all disease states—that the morphologic aspects of a disease often provide clues to its pathogenesis. It’s a visual approach. I think pathologists do tend to be very visual in their outlook.
Q: How did you get to NIH?
JAFFE: While I was doing a pathology internship at Georgetown University (in Washington, D.C.), I learned that NIH had a residency in pathology—a not-well-publicized residency; it wasn’t until moving to the area that I learned of it.
Q: What was going on in the field then?
JAFFE: I came here in 1970, and it was a time of explosive changes in the treatment of cancer at the NCI. Chemotherapy was really coming into its day and was expected to change the prognosis in many forms of cancer—in particular lymphoma, which has often been a model for treating other malignancies.
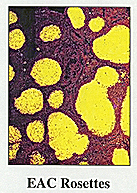
Vince DeVita and [his colleagues] were treating patients with Hodgkin’s disease and non-Hodgkin’s lymphoma. The residents had extensive exposure to hematopathology cases, and there was excitement about the clinical trials taking place. The field of immunology was also undergoing explosive growth. People were starting to dissect out the differences between T-cells and B-cells and developing tools to identify them in the laboratory and ultimately in tissue specimens. I decided to continue my training in the field by doing a fellowship here in hematopathology with Costan Berard, who was head of hematopathology at the time. He was an excellent diagnostic hematopathologist; [to strengthen our immunology base] we set up a collaboration with NIAID scientists to adapt some of the techniques that had been used in murine systems in order to identify lymphocytes in human disease. This was before the era of monoclonal antibodies, and the techniques we used—E-rosette and EAC-rosette—would be considered very primitive by today’s standards.
.Q: Could you give us a brief history of the classification system for lymphomas and how we derived the current system?
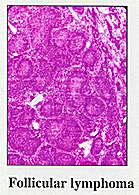
JAFFE: Historically, classification schemes by pathologists had been primarily morphologic using H&E [hematoxylin and eosin stains]. An H&E slide can give you very limited information about the disease identity. In the 1970s, people began to apply immunologic tools and concepts to the study of lymphomas—but those techniques could not be widely used, and there was a lot of controversy over lymphoma classification, with half a dozen different classification schemes being used. In 1982, the Working Formulation (WF) was published. This classification scheme was used in the U.S. until 1994, when the REAL [Revised European-American Classification of Lymphoid Neoplasms] classification was published. The WF was a purely H&E approach, proposed at a time it was thought it would not be technically feasible for pathologists to recognize T-cells and B-cells as part of daily work. Such designations were considered applicable for research only. The major drawback of the WF was that it didn’t identify disease entities. The heterogeneous categories didn’t allow pathologists and clinicians to study individual diseases in terms of their biology, natural history, or response to therapy.
 |
 |
|
|
||
Q: What advances enabled progression from the WF to the REAL?
JAFFE: Monoclonal antibody technology was developed, which permitted the generation of a huge battery of reagents that could be produced with great specificity and great consistency and from laboratory to laboratory. While the first antibodies could only be used on frozen sections, subsequent antibodies were developed that could be used on routine paraffin sections. This meant the technology could really be exported to every pathologist, whether at a major medical center or a community hospital. Also, these antibodies could be used in immunoperoxidase techniques, which allowed a permanent record.
Q: You’ve written that "The REAL classification stressed the distinction between a disease entity and a prognostic factor." What are the most important features of REAL?
JAFFE: I think the important aspect of REAL is in identifying lymphomas as individual disease entities using morphologic, immunophenotypic, and molecular tools while integrating clinical features into the definition of disease entity. For instance, in another classification system that was used extensively in Europe, what was developed for nodal lymphomas was extrapolated to extranodal lymphomas. It was assumed that a lymphoma in a lymph node and a lymphoma in the GI tract were the same. The REAL system recognized that the presentation of lymphoma in a particular anatomic site was a clue to its biology.
Q: How was REAL initiated?
JAFFE: In 1990, several European scientists decided to initiate a working group of pathologists interested in the study of lymphomas. There were 17 hematopathologists at the first meeting in London. One of the topics of discussion was mantle cell lymphoma (MCL), which at that time was not recognized as a disease entity in the WF. At NCI, it had been described as "lymphocytic lymphoma of intermediate differentiation," meaning intermediate between poorly and well differentiated. In Europe, a similar process had been called "centrocytic lymphoma." In the 1970s, we had first suggested that this lymphoma might be related to the follicular lymphoid cuff or mantle, based on morphologic and enzymatic properties. Prior to monoclonal antibodies, hematopathologists relied on the expression of certain enzymes as another way to characterize cells. We had identified alkaline phosphatase expression on the cells we called "intermediate lymphoma." Subsequently, both at NCI and in other laboratories, translocations involving the bcl-1 breakpoint region and the immunoglobulin genes were seen in these lymphomas. At the London meeting, a consensus emerged that this lymphoma was derived from mantle cells, had a characteristic immunophenotype, and had consistent genetic abnormalities. The group, now named the International Lymphoma Study Group, published a consensus paper in 1992 proposing that MCL be recognized as a distinct disease entity. Importantly, this is not just a semantic issue. The ultimate definition of MCL is not equivalent to either "intermediate lymphoma" or "centrocytic lymphoma." Biological studies have been crucial in defining the borderlines of disease entities. With this success behind us, the group started to meet every year.
Q: A progress report, of which you are first author, was recently published in the American Journal of Clinical Pathology, describing the proposed World Health Organization (WHO) classification for lymphomas. What’s the relationship between the REAL and WHO classification systems?
JAFFE: The World Health Organization publishes consensus handbooks on classification systems for all the neoplastic diseases. They hadn’t published such a classification for hematopoietic or lymphoid diseases since the 1970s. About five years ago the coordinator of the WHO classifications approached the Society for Hematopathology, of which I was then president, to help develop a new classification scheme for the WHO. Not wanting a unilateral point of view, we approached the European Association of Hematopathology to work on this with us. First, the REAL classification had been validated in clinical studies and could serve as a template for the classification of lymphomas for WHO. Second, the priniciples of the REAL could be applied to other hematopoietic malignancies. In particular, the classification of acute leukemia had not changed in 20 years and was based on an outdated scheme that did not include immunologic or genetic concepts. Just as things had changed in lymphomas, they had also changed in leukemias, with the recognition of consistent cytogenetic abnormalities in many types of leukemias that correlated with prognosis and response to therapy. The concepts of disease definition within the REAL classification were thus applied to the leukemias, to histiocytic neoplasms, and to all diseases of the hematopoietic and lymphoid systems.
Q: Just how far could we extend the principles established by the REAL classification system? Could we expect that at some point in the future, our ability to diagnose disease will become as easy as accessing a computerized spreadsheet of characteristics—your basic profile of disease?
JAFFE: Yes. I think these concepts should be applied across the board to all cancers. I think microarray technology is trying to do that and that microarrays may be the monoclonal antibodies of the future. Monoclonal antibodies are advantageous because they are broadly applicable, can be used on a large scale reproducibly, and can be applied by scientists in many different laboratories. Microarrays have the potential to take the molecular expression of a neoplasm to the next level and to produce a consistent molecular profile.
Q: Are you currently using microarray technology in your research?
JAFFE: We’ve had some collaborations with Lou Staudt [Metabolism Branch, NCI] and plan future collaborations with him in terms of applying his microarray technology of the lymphochip to the study of lymphomas. And Mark Raffeld in our group has used other types of gene expression arrays to look at lymphomas on a smaller scale.
Actually, the genetic profile of only a small number of lymphomas is very well characterized, including follicular lym phoma and mantle cell lymphoma. There are a lot of other diseases that are not as well characterized. But as the human genome is further characterized and we use microarrays and develop more tools, we will uncover the precise genetic abnormalities for most of the lymphomas and other diseases. We are learning new things every day.
Q: You’ve written that hematopathologists often serve as consultants to clinicians, patients, and other pathologists. How does educating patients and clinicians fit into your life?
JAFFE: First, let me say that one of my pet peeves is that pathologists are often misunderstood in the press. Pathologists are regarded as Dr. Death locked in the morgue. The average citizen thinks that we only do autopsies and are not really involved in a clinical situation. But in order to give the right treatment, one must have the right diagnosis, and the pathologist is critical to coming up with the right diagnosis. Pathologists can also serve as consultants to patients.
I receive a lot of cases and consultations from the outside. Patients often call me to discuss their diagnosis, the implications of their diagnosis, and what course of therapy they might choose. In a way, they regard me as a neutral consultant because I don’t have a stake in how they are going to be treated. I think the average citizen doesn’t realize that pathologists can play that role, and should play that role.
Q: What types of physicians typically seek confirmatory diagnoses? How many requests do you receive and from where?
JAFFE: I receive approximately 1,700 cases in consultation a year—about 35 a week—the majority from within the United States, but about 5 to 10 percent from other countries. In the past few months, we have received consultations from South Africa, Brazil, Argentina, England, Australia, New Zealand, Sweden, Norway, Italy, Spain, Japan, and Korea.
The cases come from both university centers and community practices. Either the pathologist who originally saw the case or the clinician taking care of the patient may seek the consultation. Sometimes pathologists on the outside have provided different diagnoses, and the physicians are trying to resolve a discrepancy.
Q: Are the samples you receive in slide form only, or do you also receive tissue samples, X-rays, ELISA data, or other diagnostic indicators?
JAFFE: A consultation case may contain anywhere from one or two slides to 50 or more slides in some complicated cases. For example, in a difficult case in which a precise diagnosis is elusive, we may receive multiple biopsies performed over a period of months to years. In nearly all cases, we receive the tissue embedded in paraffin (paraffin blocks) in addition to glass slides. The paraffin blocks are used for immunohistochemical studies, in situ hybridization, or PCR analysis of relevant DNA sequences. In some instances, we may receive either snap-frozen tissue samples or even unfixed tissue in media for more elaborate studies. The X-rays (CT scans, conventional X-rays) are sent in a small proportion of cases, but we always insist on receiving an adequate clinical history, so that we may evaluate the pathology in the clinical context.
Q: How do you proceed once samples have arrived? Do you consult with other NIH colleagues? Do you keep the samples? Do you respond formally or informally?
JAFFE: We utilize the expertise of other colleagues in evaluating the pathologic findings. We rely heavily on the ancillary laboratory services of immunohistochemistry and molecular diagnostics provided by Mark Raffeld and Lynn Sorbara of the Laboratory of Pathology (NCI). If we have viable cells, we may call upon Maryalice Stetler-Stevenson to perform flow cytometry, or cells may be provided to Diane Arthur for cytogenetic studies. Once the diagnosis is established, the patient may be referred to our clinical colleagues for admission to NIH protocols or advice about treatment alternatives. We refer many cases to Wyndham Wilson of the NCI Medicine Branch. Cases with a differential diagnosis of autoimmune lymphoproliferative syndrome will be referred to Stephen Straus (NIAID; now director of the National Center for Complementary and Alternative Medicine [NCCAM]).
We always retain representative routine slides for our files, and any immunohistochemical stains performed in our laboratory are retained in our archives. It is relatively common for us to receive additional biopsies on the same patient later, and it is important for us to be able to refer back to prior material.
We always issue a formal pathology report, which is sent to the submitting physician, and in some cases to other pathologists or clinicians involved in the patient’s care. In cases of clinical urgency, we provide an immediate verbal diagnosis over the phone.
Q: Do typical problems or inquiries regularly present themselves, or do you more often see unique cases?
JAFFE: Both. There are some regularly occurring diagnostic problems that we see often, such as the differential diagnosis between follicular lymphoma and follicular hyperplasia, or whether a biopsy is diagnostic of Hodgkin’s disease. However—especially for cases sent from other academic institutions—we often receive a case because the topic is one on which we’ve published or have a research interest. Some unique cases may lead to descriptions of new entities.
Q: Can you give us a few examples?
JAFFE: More than 10 years ago we received a number of cases that were thought to be panniculitis, or an inflammation of the subcutaneous adipose tissues. Our studies of these cases led us to conclude that this was a unique form of T-cell lymphoma, subsequently termed "subcutaneous panniculitis-like T-cell lymphoma." This rare form of lymphoma was frequently associated with a secondary syndrome in which the histiocytes (macrophages) of the patient were stimulated to undergo phagocytosis. The patients developed a fulminant hemophagocytic syndrome that was fatal in most cases.
After our publications appeared, this form of lymphoma was recognized as a distinct entity in the REAL classification and the WHO scheme. We pursued laboratory studies to try to understand the pathogenesis of the hemophagocytic syndrome that supervenes in these patients and uncovered increased expression of certain cytokines and chemokines in these tissues. More accurate diagnosis of this disease in its early stages has led to earlier and more effective therapy, improving on the clinical outlook for the patients.
Our studies have also led to new clinical protocols at NIH. For example, some years ago we were interested in trying to understand a rare type of pulmonary lymphoma, termed lymphomatoid granulomatosis. We showed that the Epstein-Barr virus played a critical role in this type of lymphoma and that many patients had underlying immune deficiencies. Through collaborations with Wyndham Wilson, new clinical protocols were developed. Wilson has shown that interferon-a can be very effective in managing many of these patients, and that they may not require aggressive chemotherapy.
Sometimes the rewards are very immediate and personal, such as making a diagnosis of Kikuchi’s disease, a benign self-limited condition, in a young woman who was about to begin chemotherapy for what was thought to be an aggressive type of lymphoma. It is especially gratifying to be able to provide such good news to a patient.
Q: Could you identify a career landmark or particular publication that catalyzed your expert status and initiated these consultations?
JAFFE: I think one’s reputation as a consultant is built gradually over many years. I enjoy teaching and lecture frequently at national and international meetings and at medical schools. In 1984, I wrote and edited a textbook on the interpretation of lymph node biopsies that became very popular.
Consultations often come about because of publications in specialized areas. Our studies showed that Hodgkin’s disease often occurred in patients with B-cell lymphoma, either in the same lymph node—so-called composite lymphoma—or sequentially with B-cell lymphomas. Because of our publications in this area, we received additional cases in consultation, enabling us to further understand this phenomenon. More recent studies from several laboratories have proven that the malignant cell of Hodgkin’s disease is B-cell in nearly all cases, in particular, a B-cell derived from the lymphoid follicle. Follicular lymphoma was the most common of lymphomas we saw in association with Hodgkin’s disease.
Q: What do you find most intriguing or challenging about your role as a worldwide advisor? Do you enjoy it?
JAFFE: In sitting down at the microscope everyday, I feel a bit like Hercule Poirot trying to solve a murder mystery. I always know I will see something challenging and interesting and that will pique my interest to try to understand it further. Diagnostic pathology is a window on the structure-function relationship of the human body. It is also fun!
About a week ago, we received
a lymph node from a patient in San Francisco with a peculiar histiocytic reaction.
The submitting pathologist was very perplexed by this process. Could it be some
bizarre infection? I recognized it as a special type of reaction seen in patients
who have received hip prostheses, and it is caused by a reaction to titanium
and cobalt-chromium found in prosthetic devices. I called the pathologist to
tell him that his patient, a 78-year-old female, must have had her hip replaced.
He checked the medical record, and indeed, the patient had received a hip replacement
six months earlier. I felt a like a psychic, and, of course, the pathologist
also was delighted to have his mystery solved. ![]()
 |
Elaine Jaffe came to NIH in 1970 and within a decade had established the reputation that mandated her presence anytime and anywhere the scientific community set about to resolve difficult issues in hematopathology. She was instrumental in the development of REAL, a classification system for identifying lymphomas adopted in 1994 and currently considered the gold standard. Her vita contains more than 400 published works (with another 13 currently pending) that have helped shape the theory and practice of her field. Her honors, awards, seats on editorial and advisory boards, society memberships, fellowships, and educational activities are—as is often said when a supremely distinguished individual is introduced at a gathering—too numerous to be listed. At NIH, she lectures to summer students and mentors hematopathology fellows. Her advice to young scientists reflects her own personal style: "Focus on a problem and finish what you start. Be committed and enjoy what you are doing. If you enjoy what you are doing, then you’re excited about it, and you’ll be successful." |